
Pelvic Floor Therapy in Cancer Care: Why It Matters
March Newsletter

Pelvic pain. Incontinence. Sexual difficulties. If you’re currently in treatment for certain types of cancers (such as cervical or prostate cancer), you may have noticed some difficult-to-discuss symptoms. And if you’re like many people – such as a recent patient of ours, Emma – you might not have realized you have options for relief.
Both cervical and prostate cancer can impact the pelvic floor, a band of muscles that supports your pelvic organs – your bladder, bowels, prostate (in men), and sexual organs (in women). Emma (not her real name) discovered this firsthand after she began experiencing a deep ache in her lower abdomen after completing treatment for cervical cancer.
Like many patients, she tried ignoring it. She told herself it would go away. But when she struggled to pick up her grandson without a sharp pain shooting through her hips, she knew she had to do something. That’s when she called Rising Sun Physical Therapy.
It was the right thing to do. Our physical therapists understand the relationship between cancer treatment and pelvic floor dysfunction and will work closely with you to find a solution that suits your needs – just as we did for Emma.
Today, we want to dive into the link between pelvic floor dysfunction and cancer and explore what we can do to help.
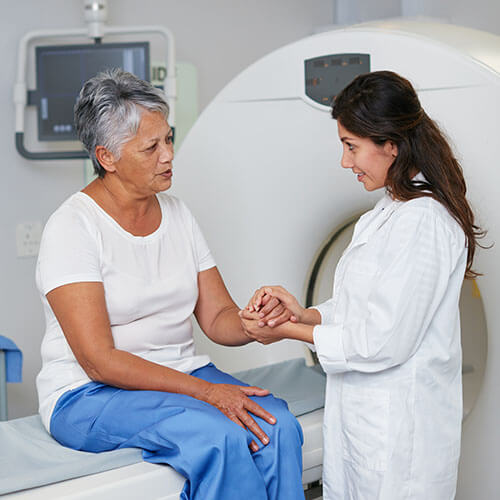
The Relationship Between Cancer and Pelvic Floor Dysfunction
Many of the treatments for cervical or prostate cancer can directly impact your pelvic floor simply due to the cancer’s location.
If you underwent surgery as part of your treatment, the procedure can affect your pelvic floor musculature or overall structure. This might happen directly, or it may result from hormonal changes that occur after the procedure.
Chemotherapy can also impact your pelvic floor, as the radiation can harden your pelvic floor muscles, which then leads to pelvic floor dysfunction and those difficult-to-discuss symptoms, like urinary or bowel incontinence, pelvic pain, or sexual dysfunction.
While we often associate pelvic floor dysfunction with women’s health, men can also experience the condition. Prostate, bladder, and anal cancer all affect men and utilize treatments that can cause difficulties in the pelvic floor.

Pelvic Floor Physical Therapy: A Path to Relief
Emma was initially hesitant to visit Rising Sun Physical Therapy. She had been through enough with treatments, doctor visits, and recovery.
However, at her first appointment, she realized physical therapy was different. Her PT explained how scar tissue, muscle tension, and weakness in her pelvic floor were making movement harder and recommended that Emma try pelvic floor physical therapy.
Pelvic floor physical therapy is a specialized type of PT that directly addresses dysfunction in the pelvic floor. Our team has extensive experience working in this area – for both men and women. As we did with Emma, we’ll work closely with you and any members of your care team to understand your specific symptoms and provide a personalized treatment plan that suits your needs.
Step 1: A Comprehensive Assessment
We always begin with a comprehensive assessment. In addition to taking a health history and learning more about your cancer treatments, we’ll perform several movement and postural screens to help us better understand how, exactly, your pelvic floor has been affected.
Step 2: A Personalized Treatment Program
Next, we pull from several treatment options to create your care plan. For Emma, we suggested gentle stretching exercises, breathing techniques, and targeted exercises to help ease the tightness in her pelvic floor and strengthen her weakened muscles.
Every program is different, however. Here are just some of the treatment methods we might suggest:
- Manual therapy techniques, such as joint mobilization or myofascial release, to help ease pain
- Visceral manipulation to help address any organ restrictions
- Lymphatic therapy to address any issues with your lymphatic system brought on by cancer treatment
- Tailored exercises to stretch and strengthen your pelvic floor muscles
- Bladder or bowel training to help manage incontinence symptoms
- Personalized education about the relationship between cancer treatments and your pelvic floor
Compassionate and Comprehensive Care
Battling cancer is hard enough. You shouldn’t also have to worry about pelvic pain and other challenging symptoms. Fortunately, our physical therapist have the expertise to ease pelvic floor dysfunction – so you can focus on what matters.
For Emma, that was being able to play with her grandkids again. What might it mean for you?
To find out, visit our website or email us at support@risingsunphysicaltherapy.com to schedule an appointment.



Our Patients Get Great Results
“This is the second time I have used Rising Sun PT and again it exceeded my expectations. Bettina worked with me this time. She not only helped improve my muscle control, but also taught me relaxation techniques that have decreased my stress levels and improved my sleep. I highly recommend the therapists at Rising Sun PT.”
—Judith W.


Integrative Wellness Partnership
Aurras Transformation offers a holistic approach to stress relief, using dance and natural rhythms to support your healing journey. Join our monthly New Moon Ritual and 5Rhythms Offerings and start your path to wellness.
Explore Our Offerings:

Bettina-Kira’s Cancer Journey
A Path to True Healing
“A single moment changed everything I believed about healing. Cancer wasn’t just a diagnosis — it was a turning point that led me to discover a deeper way to heal, beyond medicine alone. This journey shaped The Embodied Healing Continuum, showing that true healing is about reclaiming life, not just recovery.”

Aurras Waves – Dance the Breath to Your Soul
Join us weekly on Thursdays for Discover Momentum — a transformative 5Rhythms® movement experience rooted in The Embodied Healing Continuum.
This 10-session journey helps you release stress, rebuild self-trust, and reconnect with your body through movement. Guided by Bettina-Kira, it’s a space to heal, reset, and transform — one dance at a time.
Use code: RisingSun10 for 10% off (Expires April 15)
Let’s fill the space with breath, movement, and energy, building a community that dances through stress, into freedom, and back home to ourselves. Come celebrate this new beginning with me! 💃🔥


Lymphedema Risk After Cervical and Prostate Cancer
What You Need to Know
Most people associate lymphedema with breast cancer, but it can actually develop after other types of cancer, including cervical and prostate cancer.
Lymphedema develops due to disruptions in the body’s drainage of lymph fluid, leading to buildup in the surrounding tissues. It’s associated with breast cancer because two treatment options for the condition – lymph node removal and radiation therapy – can damage the lymphatic system.
However, these treatments are also used to address cervical and prostate cancer, which means it’s essential that you remain vigilant for the signs of lymphedema if you’ve undergone treatment for either one.
When It Comes to Lymphedema, Early Interaction Matters
Lymphedema develops gradually, sometimes months or even years after cancer treatment. Early symptoms are subtle, but if you do notice them early on and begin treatment immediately, you slow or even stop the progression of the condition.
Look for these early symptoms:
- Unexplained swelling in the legs, groin, or lower abdomen
- A feeling of heaviness or tightness in the affected area
- Skin changes, such as thickening or hardening
- Discomfort or aching that wasn’t there before
If you suspect you might have lymphedema, schedule an appointment at Rising Sun Physical Therapy on our website.
Our physical therapists will assess your symptoms and provide you with a personalized program to begin addressing them immediately, helping you avoid long-term complications.
Want to learn more? Visit our website to schedule an appointment.
Staff Highlight:
Bettina Neumann
Physical Therapist | Craniosacral Therapist | Lymphedema Specialist | Somatic Movement Educator | 5Rhythms® Teacher
A single moment changed everything Bettina Neumann believed about healing. Cancer wasn’t just a diagnosis — it was a turning point that led her to discover a deeper way to heal. This journey shaped The Embodied Healing Continuum, proving that true healing is about reclaiming life, not just recovery.

Meet Our Team
-

Kelsey Anderson
Operations Manager -

Bettina Neumann
PT, CST, LLCC -

Simone Vienneau
PT

Exercise of the Month
Hip Abduction (Quadruped)
Begin on all fours, with wrists directly under the shoulder and knees directly under the hips. Engage your abdominals and slowly lift one knee out to the side, keeping your knee in line with the hip. Hold as instructed, then bring your knee back down to the floor. Repeat 3 sets, 10 reps each.






Feel Better by Eating Better!
Slow Cooker White Chicken Chili
This Crockpot White Chicken Chili offers comfort and satisfaction, courtesy of its creamy texture and healthy ingredients. The slow cooker keeps it breezy and hands-free!
Place chicken in the bottom of a 6-quart or larger slow cooker. Add the chicken broth, white beans, green chiles, garlic, onion, cumin, oregano, salt, and cayenne. Stir to combine. Cover and cook on low for 4 to 6 hours or high for 2 to 4 hours, or until the chicken is cooked through. Remove the chicken breasts to a plate. Once cool enough to handle, shred and set aside.
With an immersion blender, puree a portion of the chili to thicken it, leaving some of the beans whole. (If you don’t have an immersion blender, you can instead transfer a few ladlefuls of the chili to a food processor or blender and pulse roughly, then return back into the chili.)
Stir in the shredded chicken and cilantro. Portion into bowls and top with a squeeze of fresh lime juice. Add any other desired toppings and enjoy.
Ingredients
- 1 1/4 lbs. boneless skinless chicken breasts (2-3 breasts)
- 4 cups low-sodium chicken stock
- 2 (15-oz) cans reduced-sodium white beans such as white kidney, navy, cannellini, or Great Northern beans, rinsed and drained
- 2 (4.5-ounce) cans diced green chiles
- 3 cloves garlic minced
- 1 small yellow onion (or 1/2 large) finely diced
- 2 teaspoons ground cumin
- 1 teaspoon dried oregano
- 1/2 teaspoon kosher salt
- 1/4 teaspoon cayenne pepper
- 1/4 cup chopped fresh cilantro
- Fresh lime wedges
Let’s Get You Better ASAP!
Don’t let pain dictate your life. Take the first step towards reclaiming your mobility and well-being with our expert support. Start your journey to a healthier you today.




